Christopher R. McCartney, MD
Reproductive neuroendocrinology and polycystic ovary syndrome
The long-term goal of our clinical (human subject) research is to understand the cause(s) of abnormal gonadotropin releasing hormone (GnRH) pulses and abnormal gonadotropin secretion in adolescent and adult polycystic ovary syndrome (PCOS). Specific goals of our group include elucidation of the role of progesterone in directing GnRH/LH secretion and mechanisms controlling wake vs. sleep-associated GnRH/LH pulse frequency in peripubertal girls and women, both in the presence and absence of hyperandrogenemia. Using protocols of frequent hormone sampling and formal sleep analysis, we are testing a working model that involves the primacy of sex steroid negative feedback in the control of GnRH/LH pulse frequency when awake, but the relative
hormone (GnRH) pulses and abnormal gonadotropin secretion in adolescent and adult polycystic ovary syndrome (PCOS). Specific goals of our group include elucidation of the role of progesterone in directing GnRH/LH secretion and mechanisms controlling wake vs. sleep-associated GnRH/LH pulse frequency in peripubertal girls and women, both in the presence and absence of hyperandrogenemia. Using protocols of frequent hormone sampling and formal sleep analysis, we are testing a working model that involves the primacy of sex steroid negative feedback in the control of GnRH/LH pulse frequency when awake, but the relative 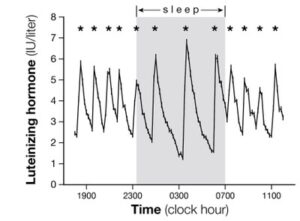 inability of sex steroids to influence GnRH/LH pulse frequency during sleep. In addition, we are pursuing studies to assess potential defects in sex steroid-mediated gonadotropin surge generation (positive feedback) in adolescents/women with hyperandrogenemia/PCOS. Moreover, we continue to pursue studies designed to elucidate mechanisms underlying obesity-associated hyperandrogenemia in peripubertal girls.
inability of sex steroids to influence GnRH/LH pulse frequency during sleep. In addition, we are pursuing studies to assess potential defects in sex steroid-mediated gonadotropin surge generation (positive feedback) in adolescents/women with hyperandrogenemia/PCOS. Moreover, we continue to pursue studies designed to elucidate mechanisms underlying obesity-associated hyperandrogenemia in peripubertal girls.
Our work is currently funded by NIH R01 HD102060 (Eunice Kennedy Shriver NICHD, “Role of Androgens in the Neuroendocrine Dysfunction of Nascent PCOS,” September 2019–June 2024).
Recent research fellows have included Su Hee Kim, MD (previously supported by NIH F32 HD088047 [2017-2018] and now supported as a faculty member by NIH K23 HD098319 [2019-2024] and Jessica Lundgren, MD (supported by NIH F32 HD091951 [2017-2019]). Although our trainees contribute to all ongoing studies, prospective new fellows could focus on one of the following areas: (1) the impact of sleep and hyperandrogenemia on sex steroid (progesterone) negative feedback regulation of GnRH pulse frequency; (2) the impact of hyperandrogenemia on estradiol- and progesterone-mediated gonadotropin surge generation (positive feedback); and (3) mechanisms underlying obesity-associated hyperandrogenemia.
